Viruses, bacteria, bugs, oh my…. pathogens that wreak havoc on our lives seems to be the topic on everyone’s mind these days. While we’re so busy dealing with COVID, it’s easy to forget about a major silent pandemic – tick-borne illnesses – that are having an increasing impact on our health.
Lyme disease, the most recognized and common tick-related infection caused by the Borrelia burgdorferi bacteria, is acknowledged in the mainstream health conversation as a pervasive threat with nearly 30,000 reported cases annually and an incidence higher than breast cancer (5). Unfortunately, new findings indicated that not only do we have to worry about Lyme, we have to consider the other multiple co-infections can be transmitted alone or in addition to borrelia, which are also on the rise. Especially as people spend more time outdoors amidst months of quarantine, Lyme and various tick-related diseases have increased as well, also complicating coronavirus pandemic detection issues in some areas such as NY state and Michigan (5).
Is it COVID…or Lyme?
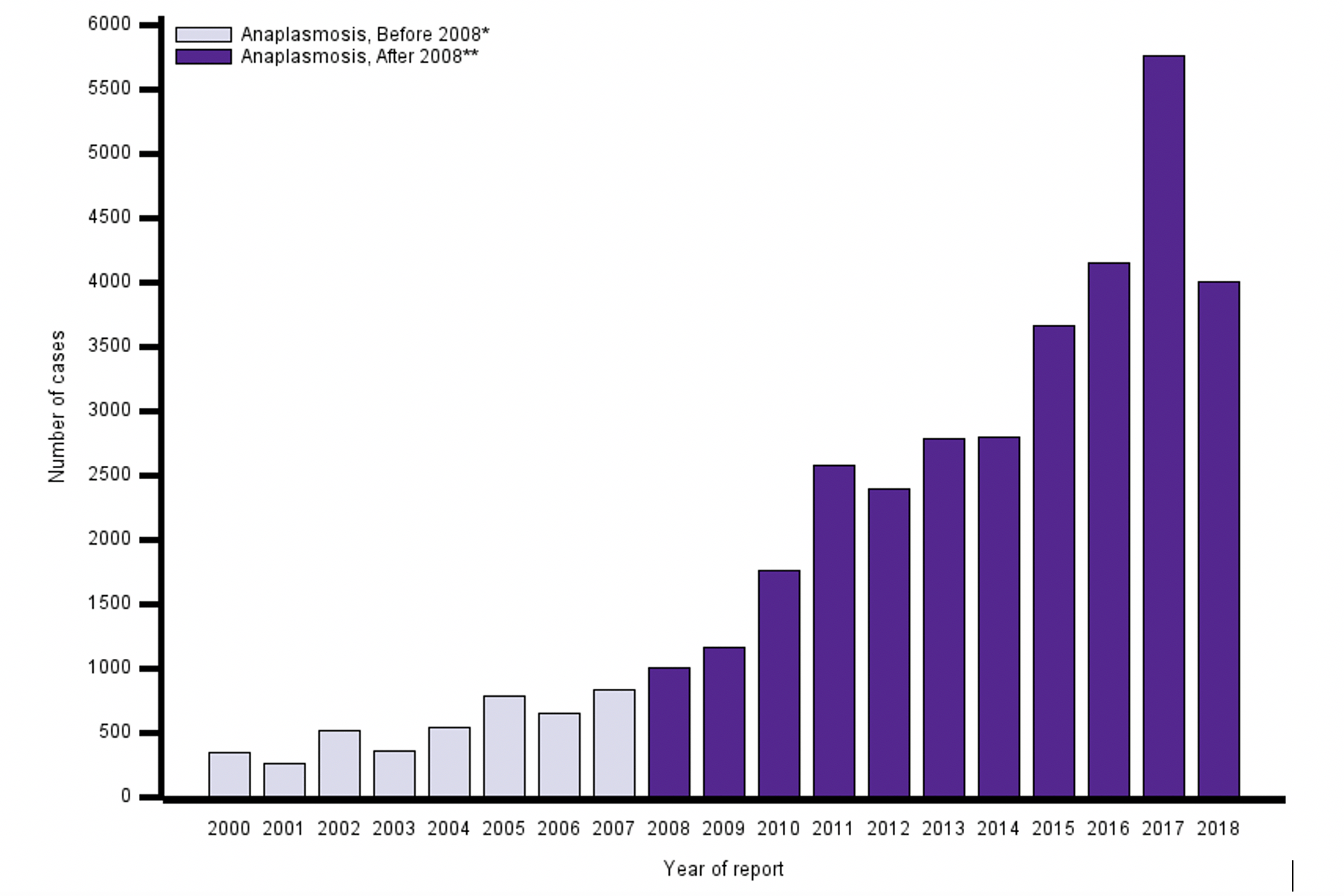
Lyme disease is a multisystem illness referred to as “the great imitator”, many times with a classic bullseye rash, flu-like symptoms, and myriad symptoms replicating conditions associated with numerous other diseases and health-impaired states, ranging from cardiac to neurological to rheumatic illnesses (5). As if we don’t have enough to worry about with COVID, more less-known tick-associated diseases are not only confusing proper diagnoses related to vector-borne illnesses, they are actually mimicking COVID symptoms in many areas. Residents in various parts of the country (such as Michigan) are seeing a growing number of anaplasmosis infection cases increase, with flu-like symptoms that easily cause COVID concern.







